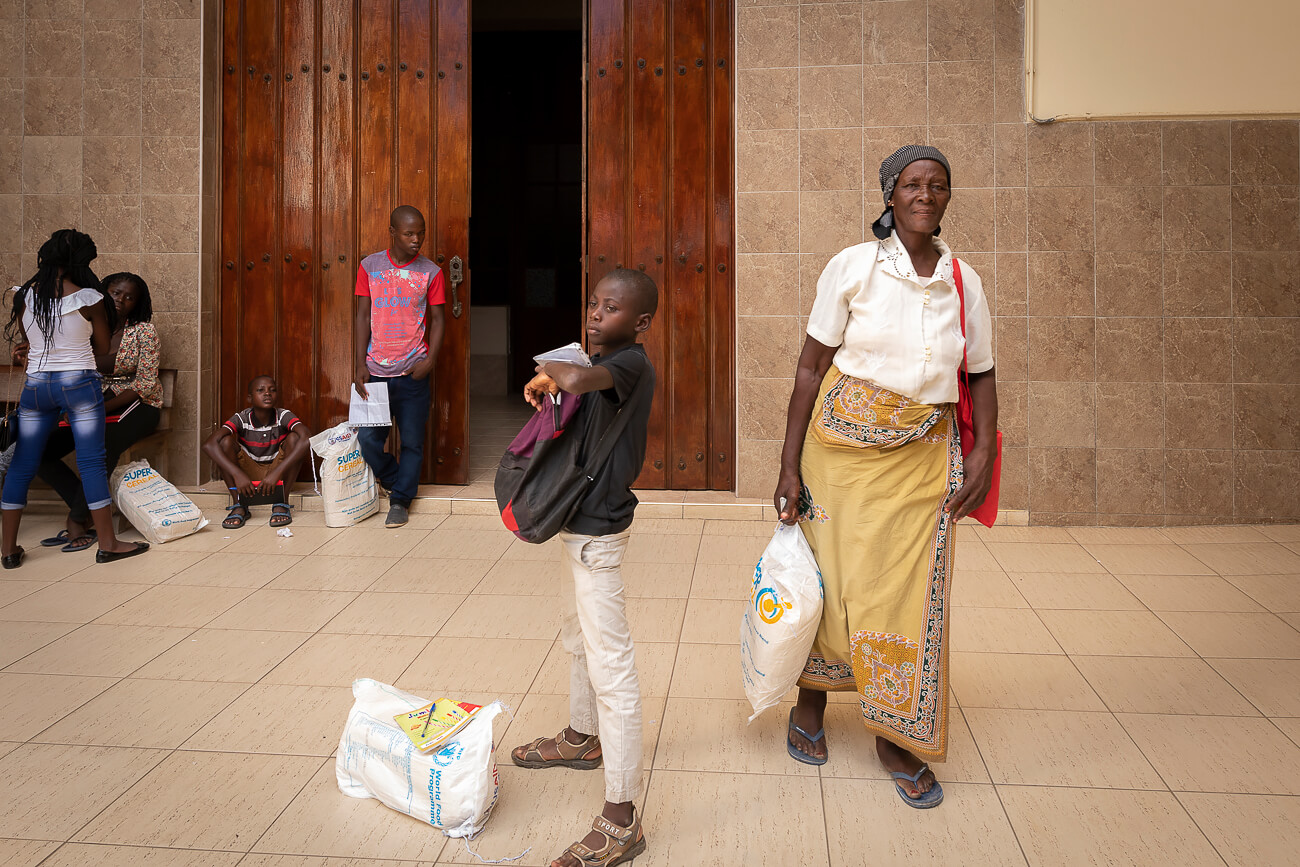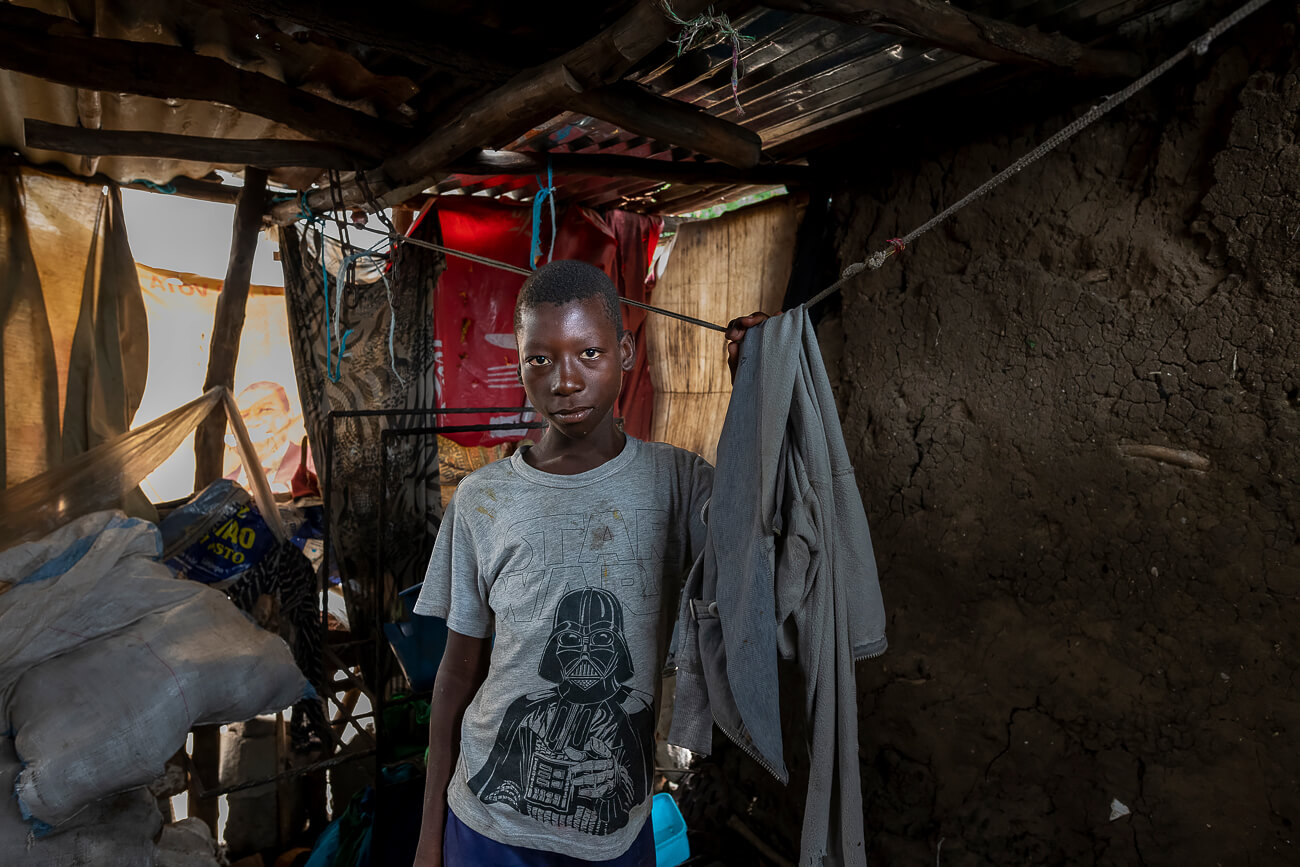What follows is a view of Mozambique from 1977 to the present through the stories of the author, who is a doctor, a hospital, and the Daughters of Charity of St. Vincent de Paoli. The story tells how a decision, which at the time seemed of minimal importance, had completely unexpected and far-reaching consequences many years later.
But this is also the story of how a lethal epidemic can be addressed when people seize an unexpected opportunity to change direction and put in place new strategies.
To work in medicine is to be a witness to both the inspiring winds of change and the rubble left behind by those for whom that change came too late.
My First Years in Mozambique - amid the war
Mozambique gained independence from Portuguese colonial rule in 1975. A civil war followed from 1977 to 1992, the impact of which included enormous loss of life and human rights violations, along with the decimation of local infrastructure including health. The war left a legacy of poverty for a large part of the population, along with a lack of health infrastructure and resources and qualified health professionals to meet the needs of individuals and communities. Public health problems, in particular HIV, tuberculosis and malaria, currently have a significant burden of disease with high mortality and morbidity rates.
When I agreed to go off to work in Mozambique, I was in my early thirties and six years into my medical career. The Health Minister of that time personally decided to send me to the town of Chokwe, where I served from 1977 until 1981 as Chief Physician of the Limpopo District in the province of Xai-Xai, Mozambique. I was the only doctor and only surgeon responsible for the care of some three hundred thousand people. I was assisted by local nurses of various origins, including two medics from Guinea Conakry and some sisters of the Daughters of Charity of San Vincenzo de Paoli.
The time I reached Chokwe, I found that reality was beyond my faintest imagination. A measles epidemic was killing and blinding children under the indifferent eyes of local nurses and nuns. Life had no meaning.
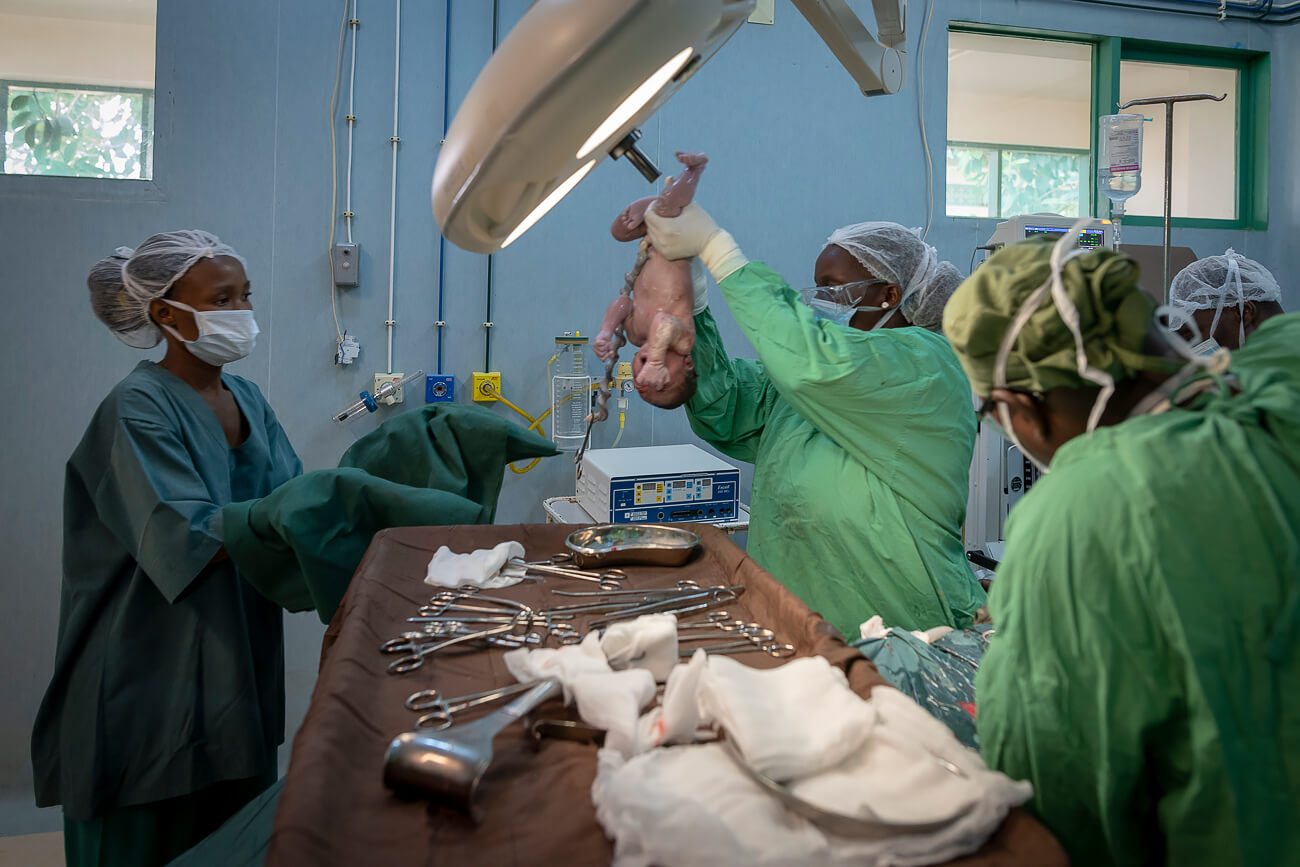
Parts of the hospital were unfinished, most importantly the operating theatre and surgery block. Rooms in the wards were filled with patients. Midwifery assistance to women delivering babies was minimal. Surgery was limited to appendicitis and cesarean sections performed by a medic from Guinea Conakry.
I got to work. I spent much of my first two years reorganizing staff responsibilities, establishing workflows, setting weekly timetables, setting protocols of treatment. At the same time, we had to finish the masonry work. All these changes came to fruition when the hospital, its staff and I had to deal with mass casualties due to military confrontation to contain a South Rhodesian attack at the Aldeia da Barragem September 1979.
The Decision
Meanwhile, in early 1979, I had asked Sister Maddalena a close collaborator to reorganize and manage the health unit in the village of Chalucuane. The village was about 60 kilometers away, but in the rainy season it remained isolated due to the lack of a good road.
Unexpectedly, this move led the Sisters to discover cases of HIV/AIDS and to envision systemic changes in district health services to fight the HIV epidemic. The move ultimately led the sisters to rethink their strategies, and to the rise of the Carmelo Hospital.
While treating tuberculosis patients in Chalucuane, Sister Maddalena and other Daughters of Charity who had come to stay with her, discovered many unjustified therapeutic failures.
It should be emphasized that in those years there was still no talk of AIDS in the country. The epidemic had begun but had not yet been recognized. Taking advantage of a donation of HIV test kits from Spain, the nuns began testing patients. They discovered an HIV seroprevalence of 30%. The combination of HIV with tuberculosis has a devastating impact on mortality and morbidity, but it also has serious social dimensions, such as the impact on family life and cohesion, economic and food security, disability and stigma. This past February, Sister Elisa was telling me ''we tried everything... but they -the AIDS patients- were just dying.''
A New Hospital
In order to deal with the emergence of the epidemic, the Sisters needed an appropriate structure. There was an abandoned convent in Chokwe, built in 1964. The nuns had been forced to leave it in 1976, one year after independence from Portuguese rule. It was returned to the Church in 1993. This building would become what is today the 125 bed Carmelo Hospital, a national reference unit for tuberculosis and HIV.
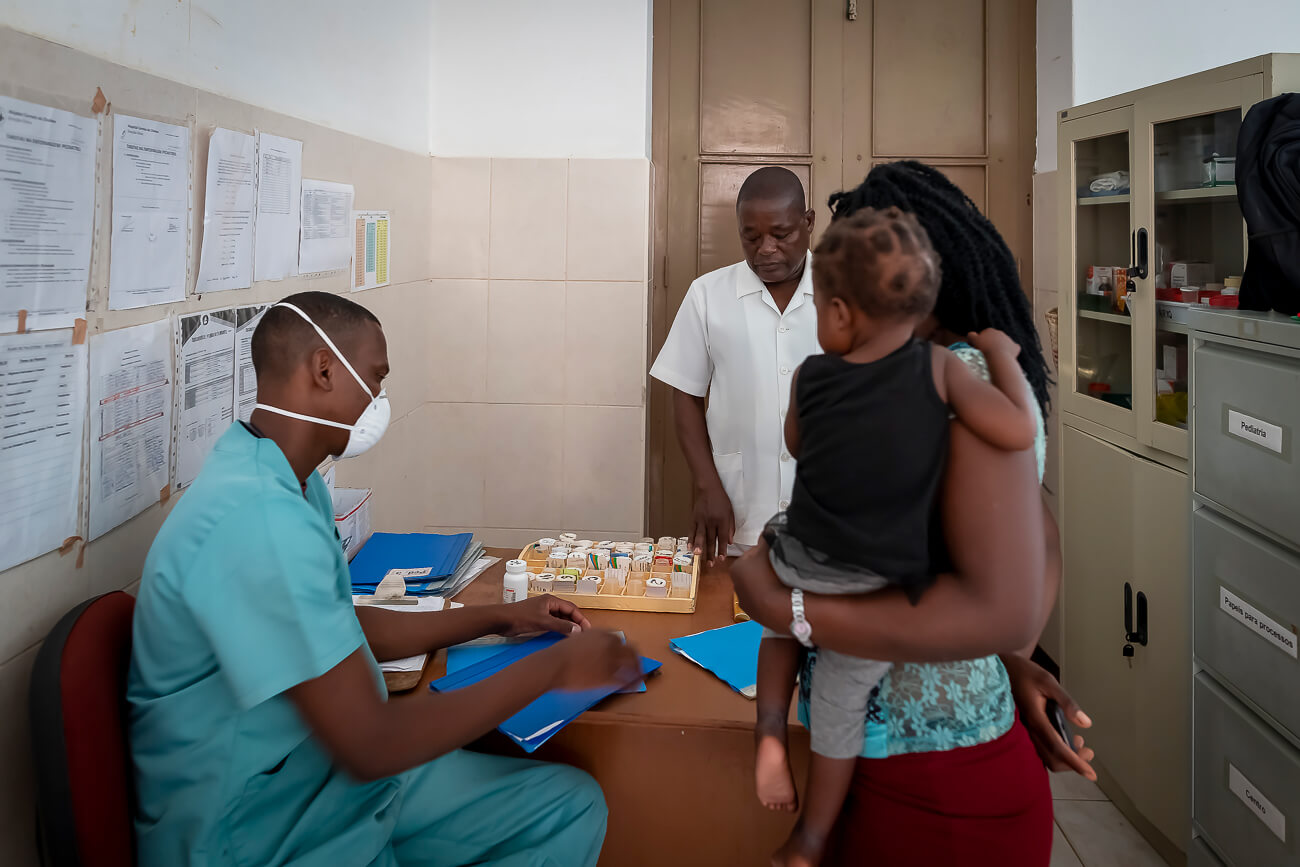
The hospital opened to its first patients on May 10, 1995. Led by the Daughters of Charity, the hospital now has Mozambican doctors, houses a sophisticated diagnostic and analysis laboratory, a bakery, a center for orphaned AIDS children and a kitchen that serves three meals a day. Hospital social workers regularly fan out to visit the families of patients in their villages to monitor the continuity of treatment and provide health support and guidance.
The Carmelo Hospital is part of the National Health system, but is run by the Daughters of Charity, a community of women who dedicate their lives to serving the poorest and most abandoned in a world fractured by poverty, social iniquity and suffering. The hospital provides care and medical assistance where it is needed. But it also ensures that orphaned children of AIDS get a family, often a grandmother, or a young relative. When needed, the hospital provides a roof, food, school supplies, and financial aid.
Solidarity and mutual assistance underpin local social structures - both within the nuclear family but also within the extended family. Everyone is responsible and cares for those in need. The nuns integrate this cultural principle through a holistic approach to individuals and the well-being of the community, regardless of the origin, religion or faith of each.
My Return to Chokwe
After more than forty years I decided to go back to Mozambique in 2019 and 2023 and entered the Carmelo Hospital for the first time. There I discovered a hospital totally dedicated to the treatment of patients with HIV/AIDS and tuberculosis, thus flanking the rural hospital where I had worked more than 40 years before.
The courtyard was crowded with hundreds of people, all waiting to undergo their first HIV test or get their monthly check-up. This was a scene I would see each day.
In the wards there were patients who suffered from AIDS and tuberculosis, but there was a human and personal touch in patient care that was evident. Given the prevalence of AIDS, the hospital has obtained authorization from the Mozambican Ministry of Health to start anti-retroviral therapy (ART) in 2002. The hospital has established first D.R.E.A.M Center (Drug Resource Enhancement against Aids and Malnutrition) - a health program created for the treatment and prevention of AIDS in Africa on the initiative of the Community of Sant’Egidio and the Dream Foundation.
Mozambique continues to be affected by the HIV epidemic. In 2023 HIV affects 11.9% of the population making it the country with the seventh highest rates of HIV in the world. For transmission of HIV from mother to child Mozambique is the second highest in the world.
In addition, there is a growing incidence of tuberculosis, which remains a huge public health challenge. This is aggravated by poverty, and lack of education for many communities that are unable to access public health information in local languages or even in Portuguese. There are currently 561 cases per 100,000 people. Only 58% of these cases have reached the health care system. About 67% of patients tested for tuberculosis are HIV positive.
The approach to the care of patients with HIV/AIDS and tuberculosis by the Daughters of Charity is to follow them from the beginning until recovery, and recognize that treating the disease alone is not enough, but that people also need practical and social support in terms of food, medicine, housing and education.
Quoting The Lancet medical journal, ''To work in medicine is to be a witness to both the inspiring winds of change and the rubble left behind by those for whom that change came too late. For today’s oncologists, infectious disease doctors, and neurologists, supporting patients relies on the knowledge that so many treatments are within reach. Medicine needs to acknowledge the wreckage of the past while also looking to the future and progress.''
The Sisters saw the beginning of the HIV/AIDS epidemic and the human wreckage it created. But they had faith that treatment would ultimately be found.
Gianni Murzi
Gianni Murzi is a doctor, who became a photographer and passionate story teller after attending seminars run by John Stanmeyer of National Geographic, then by Salwan Georges of the Washington Post and, in Rome, by Stefano Mirabella, Italian professional photographer and teacher. In his career, he worked as a surgeon in Mozambique, at the head, for four years from 1977 to 1981, of a rural hospital in the south of the country, and then moved to Zanzibar, Tanzania, as head of an Italian medical team. Subsequently joined UNICEF, the United Nations Children's Fund, over 20 years he was sent to Eastern Europe, the Middle East, South, West and North Africa, India, the United States, Iran, Albania. He now lives in Rome and travels to where photography takes him.